Pterygium surgery becomes necessary when the growth affects your vision, causes persistent discomfort, or progresses despite conservative management. In Singapore’s high-UV tropical environment, many people develop pterygium, but not everyone needs surgery. Modern conjunctival autograft techniques offer excellent outcomes with recurrence rates as low as 1.3% when combined with mitomycin C.
What Is a Pterygium?
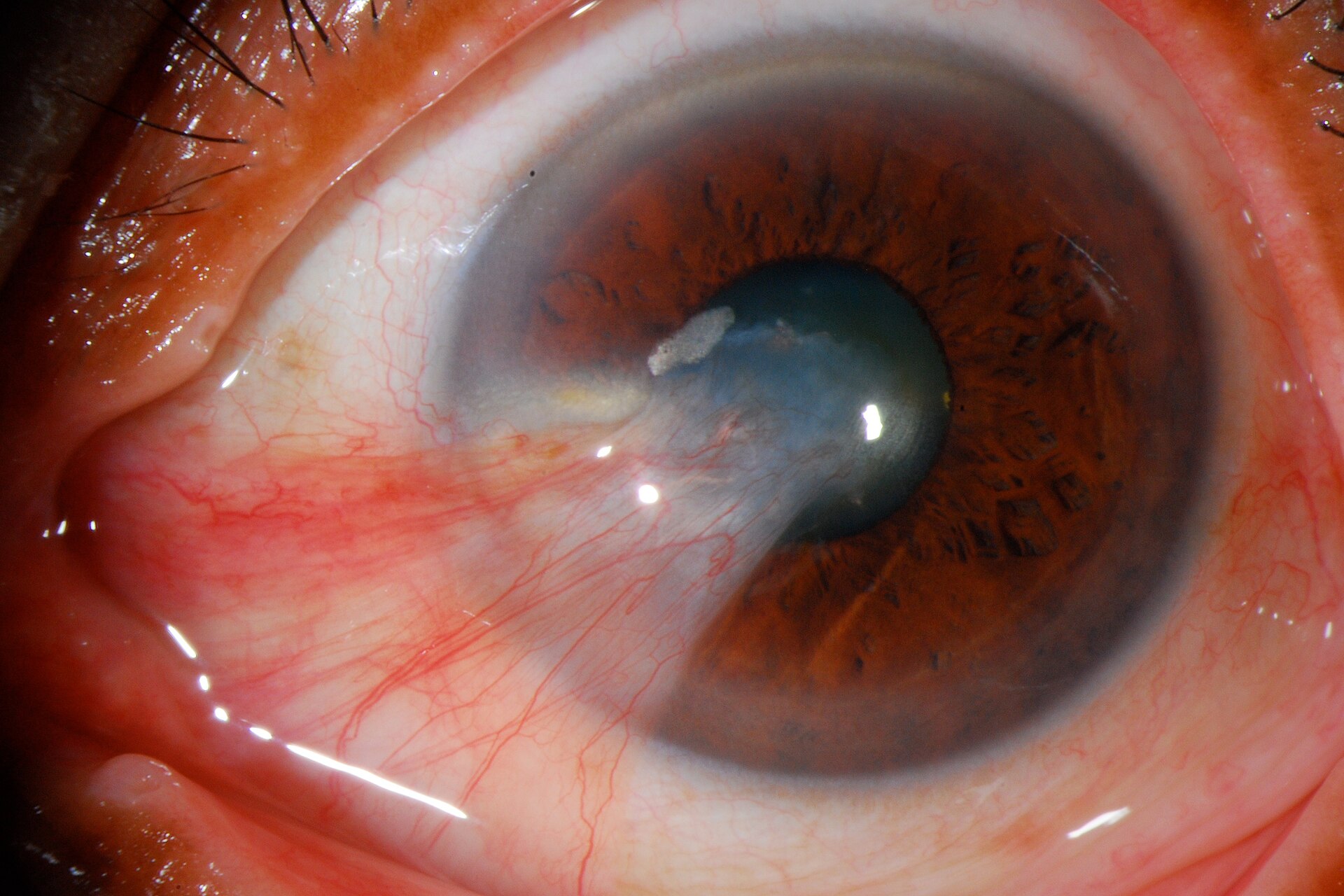
A pterygium is a benign but progressive growth of tissue on the white part of your eye that extends onto the cornea. The condition is commonly called “surfer’s eye” because it’s frequently seen in people who spend significant time outdoors. Pterygium develops when prolonged UV exposure triggers abnormal tissue growth, and it’s particularly common in tropical regions like Singapore where UV intensity is consistently high throughout the year.
In Singapore, the UV index regularly reaches extreme levels (11 and above at midday), with no seasonal variation. This constant exposure explains why pterygium prevalence is significantly higher in our population compared to temperate climates. Outdoor workers, construction labourers, and those engaged in regular outdoor activities face four to five times higher risk of developing pterygium than desk-based workers. Even National Service conscripts who participate in field training sometimes develop the condition more rapidly due to intensive sun exposure.
The growth typically starts on the inner side of your eye (near your nose) and gradually extends across the cornea. While some people have no symptoms, others experience redness, irritation, dryness, a gritty sensation, or tearing. As the pterygium progresses, it can induce astigmatism and blur your vision, particularly if it extends into the visual axis.
Non-Surgical Management Options
If you’ve been diagnosed with pterygium, surgery isn’t always the first step. Conservative management is appropriate when the growth isn’t affecting your vision and symptoms are minimal. Understanding your non-surgical options helps you make an informed decision with your eye specialist.
Protective eyewear is fundamental to halting pterygium progression. Wearing quality sunglasses with 100% UV protection and wide coverage (or wraparound styles) significantly reduces further UV damage and can slow growth. UV protection alone can reduce pterygium incidence by 50 to 70%, making this a highly effective first-line strategy in Singapore’s intense outdoor environment.
Artificial tears and lubricating eye drops address the dryness and irritation that often accompany pterygium. These drops don’t shrink the growth, but they improve comfort and reduce inflammation. If standard artificial tears aren’t sufficient, your eye specialist might prescribe medicated drops containing anti-inflammatory agents to manage redness and discomfort. Drops work best for symptomatic relief rather than halting progression.
Regular monitoring is essential when you choose conservative management. Your eye specialist will schedule periodic examinations to track the pterygium’s size, assess any changes in your vision, and evaluate whether symptoms are worsening. If the growth stabilises without affecting vision, ongoing conservative care remains appropriate. Many patients live comfortably with pterygium that isn’t progressive or visually significant.
When Surgery Becomes Necessary
Surgery becomes necessary when pterygium interferes with your quality of life or vision. The primary indications for pterygium removal include vision impairment from the growth extending into your visual axis, significant astigmatism induction, persistent redness and discomfort unresponsive to drops, and cosmetic concerns.
Vision impairment is the most common surgical indication. If pterygium has extended far enough onto your cornea that it’s blurring your sight, surgical removal restores clarity. Even mild blur can significantly affect daily activities, and corrective lenses cannot adequately compensate for pterygium-induced astigmatism. Your eye specialist uses specific measurements during examination to determine whether the growth is affecting your visual axis.
Persistent discomfort is another important consideration. Some patients develop chronic irritation, redness, or a foreign body sensation that doesn’t improve with drops or sun protection. If you’ve tried conservative measures for a reasonable period and continue experiencing significant discomfort, surgery offers definitive relief.
Progressive growth despite UV protection suggests the pterygium has developed aggressive characteristics. If your eye specialist observes rapid advancement, increasing astigmatism, or documented growth on serial measurements, surgical intervention prevents further encroachment onto your cornea. Acting before the growth severely affects vision produces better visual outcomes.
Pterygium Surgery in Singapore — What to Expect
Modern pterygium surgery has evolved significantly from older methods, with current approaches achieving recurrence rates below 5% in most cases. The gold-standard technique is conjunctival autograft surgery, where the surgeon removes the pterygium and grafts healthy conjunctival tissue (from elsewhere on your eye) to cover the area.
A recent meta-analysis of over 5,000 eyes across 21 randomised controlled trials demonstrates that conjunctival autograft alone achieves approximately 3% recurrence, while adding mitomycin C (MMC) — an anti-scarring agent — reduces recurrence to just 1.3%. This compares favourably to the older bare sclera technique, which had recurrence rates of 40–50%.
During your surgery, your eye specialist administers local anaesthesia, so you’re awake but comfortable. The surgeon carefully removes the pterygium and any abnormal tissue, then harvests conjunctival tissue and secures it with either sutures or fibrin glue. Fibrin glue application has become increasingly popular because it reduces tissue trauma and healing time, with 2% recurrence rates at 12 months compared to 8% with sutures. The entire procedure typically takes 20 to 40 minutes.
Recovery is relatively quick. Most patients notice improved comfort within the first few days. You’ll use antibiotic and anti-inflammatory eye drops for several weeks, and your vision gradually stabilises over one to two months. Some mild discomfort, tearing, and redness in the immediate post-operative period are normal. Avoiding strenuous activity, swimming, and dusty environments for two to four weeks protects your healing graft.
A significant benefit of modern surgery is rapid astigmatism reduction. Many patients experience one to two diopters of astigmatism improvement after pterygium removal, often noticing sharper vision within weeks. Cosmetic results are excellent in over 95% of cases, with the eye returning to a natural appearance.
Post-operative care is crucial for preventing recurrence. Even after successful surgery, consistent UV protection with sunglasses significantly reduces the risk of pterygium returning. Your eye specialist will emphasise continued sun protection as a lifetime habit, and regular follow-up appointments monitor for any signs of recurrence.
For more information about eye surgeries available at IECRC, speak with our specialist team.
Frequently Asked Questions
Can pterygium be treated with eye drops without surgery?
Pterygium itself cannot be reversed with eye drops alone. However, drops are extremely useful for managing symptoms while the pterygium remains stable. If you have mild redness, irritation, or dryness, lubricating drops and anti-inflammatory medications can provide significant relief. The key limitation is that drops don’t stop the growth or prevent progression; they address discomfort while conservative management continues. If your pterygium is asymptomatic and not progressing, drops combined with UV protection may be all you need. However, if symptoms persist despite adequate drop therapy or if the pterygium is expanding, surgery becomes the appropriate next step.
How long does it take to recover from pterygium surgery?
Most patients experience rapid initial improvement, with noticeably increased comfort within the first week. You can resume light daily activities within one to two weeks, though you should avoid strenuous exercise, swimming, and dusty environments for at least four weeks. Your vision usually stabilises within six to eight weeks, though some continued gradual improvement may occur over several months. Full graft integration and maximum astigmatism reduction typically take two to three months. During this period, you’ll use prescribed eye drops and attend follow-up appointments to monitor healing.
Is pterygium surgery covered by MediSave and/or Insurance in Singapore?
Pterygium surgery may be eligible for MediSave and/or Insurance claims if the procedure is deemed medically necessary — meaning it’s affecting your vision or causing significant symptoms — rather than purely cosmetic. Coverage depends on your individual circumstances and the specific guidelines at the healthcare institution where you’re having surgery. We recommend discussing MediSave.Insurance eligibility with your eye specialist during your consultation, as they can provide specific information about what portions of the procedure might qualify for MediSave/Insurance claims.
Can pterygium come back after surgery in Singapore’s climate?
Yes, pterygium can recur after surgery, though modern techniques have dramatically reduced recurrence rates. With conjunctival autograft surgery combined with mitomycin C, recurrence occurs in approximately 1.3% of patients — a major improvement over older techniques. Singapore’s intense year-round UV exposure does present an ongoing risk, particularly if sun protection measures are neglected. The most effective prevention strategy is consistent use of UV-blocking sunglasses and limiting prolonged midday sun exposure. Many patients find that maintaining these protective habits indefinitely prevents recurrence, and regular eye examinations help detect early recurrence if it begins.
References:
Singapore UV index and pterygium risk. Singapore Uncensored.
Conjunctival autograft and fibrin glue in pterygium surgery. Cureus.
Pterygium management guidelines. Greenwich Eye.
Last reviewed: March 2026
Medically reviewed by Dr Joy Chan, Medical Director & Senior Consultant
Disclaimer: This article is for general informational purposes only and does not constitute medical advice. Please consult an ophthalmologist for personalised guidance.