Eye Lens (Crystalline Lens): Understanding Your Eye's Natural Focusing System
The lens of your eye is a transparent structure that functions like a camera lens to help you see clearly at varying distances. Located just behind the colored iris, this clear, flexible component automatically adjusts its shape to focus light onto the retina at the back of your eye. When you look at something close, like a book, or far away, like a bird in the sky, your lens changes shape to keep the image sharp. While this natural focusing system works for most of your life, changes to the lens over time can affect your vision and may require professional care.
Important: All lens treatments and surgeries carry risks. This information is educational and should not replace individual consultation with a qualified ophthalmologist.
Understanding the Eye Lens
The eye lens, also called the crystalline lens, is a clear, biconvex structure embedded within your eye that plays a role in vision. It sits directly behind your pupil and is held in place by tiny elastic fibers called zonules, which connect to the ciliary body, a ring of muscle tissue surrounding the lens.
Your lens is composed of specialized transparent proteins called crystallins, which provide clarity and focusing power. Unlike most cells in your body, lens cells do not regenerate or replace themselves. Instead, new cells continuously form at the outer edges throughout life, while older cells compress toward the center in concentric layers, similar to tree rings.
How the Lens Functions
The primary function of your eye lens is to fine-tune focus by bending incoming light rays toward a single point on the retina. While your cornea provides approximately 70% of your eye's focusing power, the lens contributes the remaining 30%. What makes the lens unique is its ability to change shape through a process called accommodation.
When you look at distant objects, the ciliary muscles relax, causing the zonules to pull on the lens capsule and flatten the lens. When viewing nearby objects, the ciliary muscles contract, the zonules relax, and the lens becomes more rounded and curved. This automatic adjustment happens instantaneously and allows you to shift focus between different distances throughout the day without conscious effort.
Anatomy and Position
The lens measures approximately 10 millimetres in diameter and 4 millimetres in thickness, though this varies with accommodation. It is completely transparent and has no blood vessels or nerve fibers running through it, which is essential for maintaining clarity. The lens is surrounded by a thin, elastic capsule that protects it and allows shape changes during accommodation.
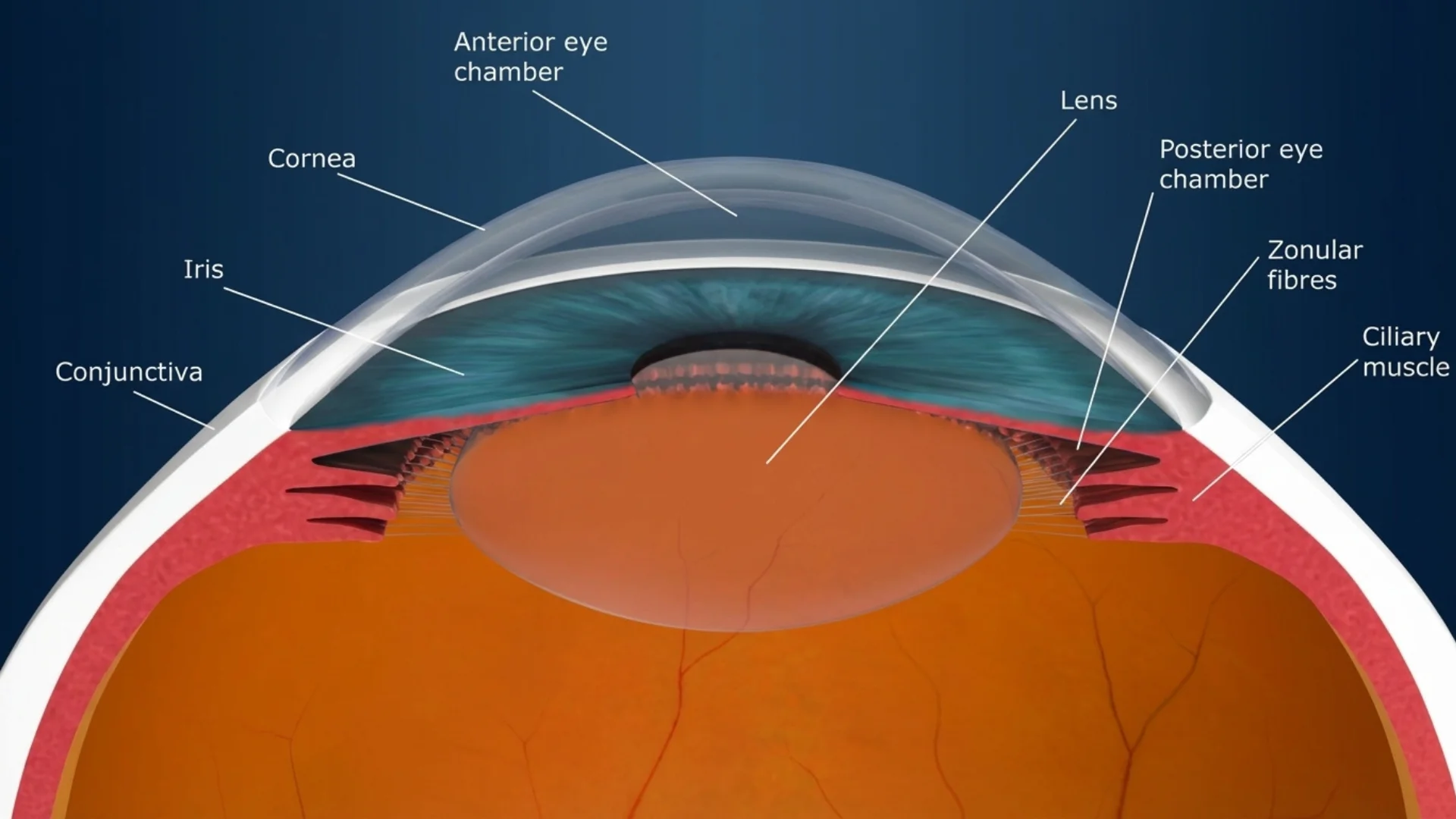
Located in the anterior segment of the eye, the lens divides the eye into two chambers: the anterior chamber between the cornea and lens filled with aqueous humor, and the posterior chamber behind the lens filled with vitreous humor. This strategic position allows it to receive light that has already been partially focused by the cornea and refine that focus before the light reaches the retina.
Common Lens-Related Conditions
Cataracts
Cataracts occur when the normally clear lens becomes cloudy or opaque, causing blurred or dimmed vision. This is the most common condition affecting the lens and is primarily age-related. As crystallin proteins break down and clump together over time, they create cloudy areas that scatter light and reduce visual clarity. The cloudiness typically starts small and gradually expands, though progression rates vary among individuals.
Beyond aging, several factors can contribute to cataract development including prolonged ultraviolet radiation exposure from sunlight, smoking and secondhand smoke exposure, poorly controlled diabetes, previous eye injuries or inflammation, long-term corticosteroid use, and genetic factors or congenital conditions present at birth. Research published in the American Journal of Epidemiology has shown that UV exposure significantly increases cataract risk over time.
Common symptoms include cloudy or blurred vision, increased sensitivity to glare especially from headlights at night, seeing halos around lights, faded or yellowed colors, difficulty with night vision, and frequent changes in glasses or contact lens prescription. While cataracts do not cause pain, they significantly impact quality of life when they interfere with daily activities such as reading, driving, or recognizing faces.
Presbyopia
Presbyopia is an age-related condition affecting everyone, typically becoming noticeable after age 40. As the lens ages, it gradually loses flexibility and ability to change shape effectively. The proteins that give the lens its elastic properties become stiffer, and the ciliary muscles that adjust the lens also weaken with age.
This natural aging process makes it increasingly difficult to focus on nearby objects. You may find yourself holding reading materials farther away to see them clearly, experiencing eye strain or fatigue when reading or doing close work, needing brighter lighting for near tasks, or having difficulty switching focus between near and far distances.
Unlike myopia or hyperopia, which are refractive errors present from earlier in life, presbyopia is universal and progressive. It continues to worsen gradually until around age 65, when the lens loses nearly all remaining flexibility. Studies in Investigative Ophthalmology & Visual Science have documented the biomechanical changes in the aging lens that lead to presbyopia.
Lens Dislocation
Although less common, the lens can become displaced from its normal position if the zonules holding it in place are damaged or weakened. This condition, called lens dislocation or ectopia lentis, can result from trauma to the eye, genetic connective tissue disorders such as Marfan syndrome, severe myopia, or previous eye surgery complications.
A displaced lens can cause sudden vision changes, double vision in one eye, significant refractive error changes, or in severe cases complications such as glaucoma or retinal detachment. Lens dislocation requires prompt evaluation and treatment by an ophthalmology specialist to prevent further complications.
Diagnostic Procedures for Lens Conditions
Accurate diagnosis of lens-related conditions requires comprehensive eye examinations performed by qualified eye care professionals. Our comprehensive eye examination services utilize advanced diagnostic technology to assess lens clarity and function.
Visual Acuity Testing
Visual acuity testing measures how well you can see at various distances. You will be asked to read letters or numbers of decreasing size on a standardized eye chart placed at a specific distance. This fundamental test helps identify vision problems that may result from lens conditions and provides a baseline for tracking changes over time.
Slit Lamp Examination
A slit lamp is a specialized microscope with a bright light source that allows your ophthalmologist to examine the structures at the front of your eye, including the lens, in great detail. During this examination, your doctor can detect early cataract formation, assess the degree of lens cloudiness, evaluate lens capsule integrity, and identify any signs of lens displacement or inflammation.
Refraction Assessment
Refraction testing determines the precise corrective lens prescription needed to optimize your vision. During this procedure, your eye doctor uses various lenses and a phoropter to measure how light bends as it enters your eye. This assessment is crucial for identifying refractive errors and determining whether vision problems stem from the lens or other eye structures.
Dilated Eye Examination
For thorough evaluation of the lens and other internal eye structures, your ophthalmologist will instill dilating drops that temporarily enlarge your pupils. Once dilated, they can examine the entire lens, including the posterior capsule and peripheral areas not visible through an undilated pupil. This examination is essential for detecting subtle cataracts, assessing lens positioning, and evaluating retinal health behind the lens.
Optical Biometry
When cataract surgery or refractive lens exchange is being considered, optical biometry measures the length of your eye and corneal curvature. These precise measurements are critical for calculating the power of the intraocular lens that will replace your natural lens, ensuring optimal vision outcomes after surgery. Clinical studies in the Journal of Cataract & Refractive Surgery have established the importance of accurate biometry for surgical success.
Treatment and Surgical Procedures
Cataract Surgery
Cataract surgery is a treatment that removes a cloudy lens. It is one of the commonly performed surgical procedures, though all surgery carries risks that should be carefully considered before proceeding.
Risks of Cataract Surgery: All surgical procedures carry risks including infection, bleeding, retinal detachment, increased eye pressure, lens fragments remaining in the eye, vision loss, inflammation, and in rare cases permanent blindness. Some patients may experience posterior capsule opacification requiring laser treatment. Additional surgery may be needed in some cases. All risks should be discussed with your ophthalmologist before proceeding.
The Phacoemulsification Procedure
Modern cataract surgery typically uses a technique called phacoemulsification. During this procedure, which usually takes 30 to 60 minutes, your surgeon makes a small incision in the cornea. Using an ultrasound probe, they break up the cloudy lens into tiny fragments and remove them. The posterior capsule, the back part of the lens covering, is left intact to support the artificial lens.
Your surgeon then inserts a folded intraocular lens through the small incision. Once inside the eye, the IOL unfolds and is positioned where your natural lens was located. The incision is typically self-sealing and requires no stitches in most cases.
Cataract surgery is performed as a day procedure, meaning you return home the same day. A mild sedative and local anesthetic eye drops are used. Some patients may experience discomfort, and vision improvement timeline varies by individual.
Intraocular Lens Options
Several types of IOLs are available, each with different characteristics.
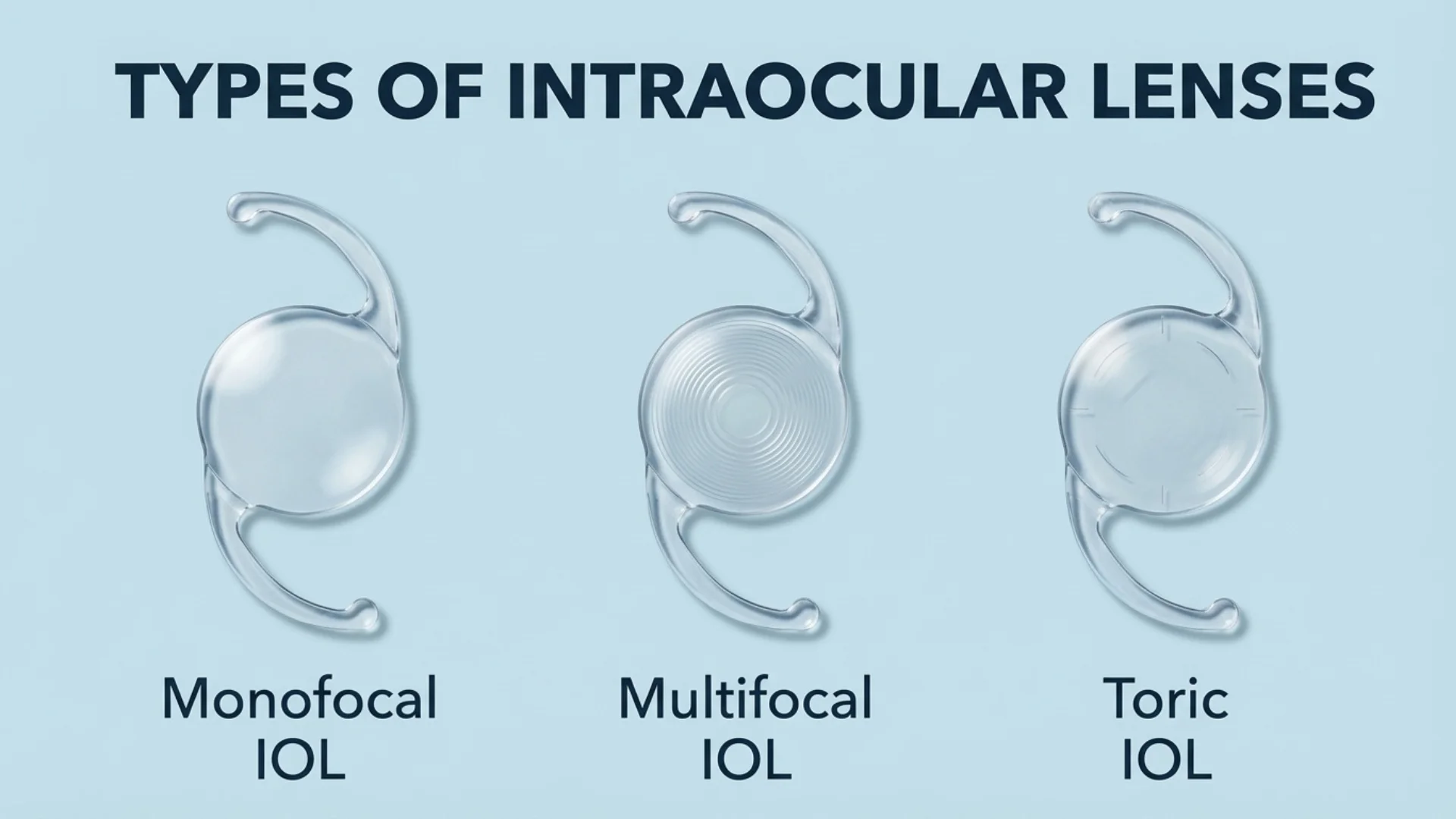
Monofocal IOLs provide vision at one distance, usually far, though you will likely need reading glasses for close work. Multifocal IOLs have multiple zones designed to provide vision at various distances, though some patients may experience glare, halos, or reduced contrast sensitivity. Toric IOLs correct astigmatism in addition to cataracts. Extended depth of focus IOLs provide a range of vision, though visual outcomes vary by individual.
During your pre-surgical consultation, your ophthalmologist will discuss which IOL type may be suitable for your situation, along with the specific risks and limitations of each option. Research in Ophthalmology journals continues to evaluate outcomes with different IOL technologies.
Refractive Lens Exchange
For patients over 50 who have significant refractive errors that exceed the range suitable for laser vision correction, refractive lens exchange offers an alternative. This procedure is essentially the same as cataract surgery but is performed on a clear lens to correct vision rather than treat cataracts.
RLE can correct severe myopia, hyperopia, or astigmatism while simultaneously preventing future cataract development, since the natural lens is replaced with a clear artificial one. The procedure, recovery, and lens options are identical to those used in cataract surgery.
Presbyopia Correction Options
While presbyopia cannot be reversed, several effective treatment options can restore functional near vision.
Reading Glasses or Bifocals
The simplest and most common solution involves wearing reading glasses when performing close tasks. Bifocal or progressive lenses can be incorporated into your regular glasses, providing seamless transition between distance and near vision correction.
Contact Lenses
Specialized contact lenses designed for presbyopia include multifocal contact lenses that work similarly to multifocal spectacle lenses, and monovision correction where one eye is corrected for distance and the other for near vision. While monovision reduces depth perception slightly, many people adapt well to this approach.
Refractive Surgery
For those seeking spectacle independence, several surgical options exist. Monovision LASIK creates the same effect as monovision contact lenses but through permanent corneal reshaping. Alternatively, refractive lens exchange with multifocal or EDOF IOLs can provide comprehensive presbyopia correction while preventing future cataracts.
Post-Operative Care and Recovery
Following any lens surgery, proper care is essential for optimal healing and outcomes.
Immediate Post-Operative Period
You will receive antibiotic and anti-inflammatory eye drops to prevent infection and reduce inflammation. Use these exactly as prescribed, maintaining proper hand hygiene before administering drops. An eye shield may be provided to wear while sleeping for the first week to protect your eye from accidental rubbing or pressure.
Avoid getting water directly in your operated eye for at least one week. You may shower and wash your face, but do so carefully to prevent water, soap, or shampoo from entering your eye. Avoid swimming, hot tubs, and water sports for at least two weeks following surgery.
Activity Restrictions
Most daily activities can resume within a few days, though you should avoid strenuous exercise, heavy lifting over 10 kilograms, and activities that might risk eye injury for at least two weeks. Gentle walking is encouraged, but hold off on running, contact sports, or yoga positions where your head is below your waist.
You may experience mild discomfort, light sensitivity, or fluctuating vision during the first few days, which is normal. However, if you experience severe pain, sudden vision loss, increasing redness, or flashing lights and floaters, contact your ophthalmologist immediately, as these could indicate complications requiring urgent attention.
Preventive Care and Lens Health Maintenance
While age-related changes to the lens are inevitable, several lifestyle measures can help maintain lens clarity and delay cataract formation.
UV Protection
Ultraviolet radiation from sunlight is a significant risk factor for cataract development. Wear sunglasses that block 100% of UVA and UVB rays whenever you are outdoors, even on cloudy days. Wide-brimmed hats provide additional protection by reducing the amount of sunlight reaching your eyes from above. World Health Organization guidelines emphasize the importance of UV protection for eye health.
Smoking Cessation
Smoking significantly increases the risk of early cataract formation and progression. If you smoke, quitting is one of the most important steps you can take to protect your vision. Avoid secondhand smoke exposure as well, as it also contributes to lens damage. Research in the British Medical Journal has documented the strong association between smoking and increased cataract risk.
Diabetes Management
Poorly controlled blood sugar levels accelerate cataract development and can cause temporary refractive changes that affect vision. If you have diabetes, work closely with your healthcare team to maintain stable blood glucose levels through medication, diet, and lifestyle modifications. Regular comprehensive eye examinations are particularly important for people with diabetes.
Nutrition
While no specific dietary supplement has been proven to prevent cataracts, a diet rich in antioxidants may support overall eye health. Include plenty of colorful fruits and vegetables, particularly leafy greens, which contain lutein and zeaxanthin. These nutrients concentrate in the lens and may help protect against oxidative damage. Studies published in Archives of Ophthalmology have examined the relationship between nutrition and lens health.
Regular Eye Examinations
Routine eye examinations allow for early detection of lens changes before they significantly impact your vision. Adults over 40 should have comprehensive eye exams every one to two years, while those over 60 or with risk factors should have annual examinations. Children should receive vision screening at regular intervals to detect conditions such as congenital cataracts or amblyopia that can affect visual development.
When to Seek Professional Care
Schedule a comprehensive eye examination with our ophthalmology specialists if you experience gradual or sudden changes in vision clarity at any distance, increasing difficulty reading or performing close work, noticeable glare, halos around lights, or light sensitivity, frequent changes in your glasses or contact lens prescription, cloudy or hazy vision that affects daily activities, double vision in one eye, or difficulty with night driving or distinguishing colors.
Early intervention can prevent vision loss and improve quality of life. Many lens-related conditions develop gradually, making regular eye examinations essential for detecting changes before they significantly impact your daily activities.
Conclusion
The crystalline lens is a component of your visual system, providing focusing adjustments for vision at different distances. Understanding lens-related conditions, recognizing symptoms early, and seeking timely professional care are important for managing vision throughout life. Various diagnostic techniques and treatment options are available for lens conditions.
Important Medical Notice: This information is for general educational purposes and does not replace professional medical advice. Lens conditions vary in severity and treatment requirements. For personalized assessment and treatment recommendations, please schedule a consultation with our eye care specialists. All surgical procedures carry risks including infection, bleeding, vision loss, retinal detachment, glaucoma, inflammation, and in rare cases permanent blindness. All risks, benefits, and limitations should be thoroughly discussed with a qualified ophthalmologist before proceeding with any treatment.
Licensed Healthcare Service: For questions about our services or to book an appointment, please visit our contact page or call our clinic during operating hours. For medical emergencies, please contact emergency services immediately.
When to Seek Professional Care
Clouding of the eye's natural lens reduces visual clarity and causes glare, progressing gradually with age but treatable through surgical lens replacement to restore clear vision. Please visit the doctor if you have any of the following symptoms:
Increasingly cloudy or hazy vision affecting daily tasks
Heightened glare sensitivity especially from vehicle headlights
Colours appearing faded yellowed or less vibrant
Difficulty seeing clearly at night or low light
Frequent prescription changes despite corrective lenses
Early assessment by an ophthalmologist allows timely intervention, preserves quality of life, and prevents further deterioration through appropriate lens treatment options.

